Articles
- Page Path
- HOME > J Korean Acad Nurs > Volume 56(1); 2026 > Article
-
Research Paper
통합간호역량 향상을 위한 간호교육의 전환: 증상 기반 임상추론에 대한 델파이 방법론 연구 -
김증임1,*
 , 유소영2,*
, 유소영2,* , 박진희3
, 박진희3 , 송주은3
, 송주은3 , 류은정4
, 류은정4 , 이주희5
, 이주희5 , 임여진6
, 임여진6
- Transforming nursing education to enhance integrated nursing competency: a Delphi-based methodological study on symptom-based clinical reasoning
-
Jeung-Im Kim1,*
 , Soyoung Yu2,*
, Soyoung Yu2,* , Jin-Hee Park3
, Jin-Hee Park3 , Ju-Eun Song3
, Ju-Eun Song3 , Eunjung Ryu4
, Eunjung Ryu4 , JuHee Lee5
, JuHee Lee5 , YeoJin Im6
, YeoJin Im6
-
Journal of Korean Academy of Nursing 2026;56(1):39-50.
DOI: https://doi.org/10.4040/jkan.25151
Published online: February 5, 2026
1순천향대학교 의과대학 간호학과
2차의과학대학교 간호대학
3아주대학교 간호대학ㆍ간호과학연구소
4중앙대학교 적십자간호대학
5연세대학교 간호대학ㆍ김모임간호학연구소
6경희대학교 간호과학대학
1School of Nursing, Soonchunhyang University College of Medicine, Cheonan, South Korea
2College of Nursing, CHA University, Pocheon, South Korea
3College of NursingㆍResearch Institute of Nursing Science, Ajou University, Suwon, South Korea
4Red Cross College of Nursing, Chung-Ang University, Seoul, South Korea
5College of NursingㆍMo-Im Kim Nursing Research Institute, Yonsei University, Seoul, South Korea
6College of Nursing Science, Kyung Hee University, Seoul, South Korea
- Corresponding author: YeoJin Im College of Nursing Science, Kyung Hee University, Rm# 412, SPACE 21 Bldg., 26 Kyungheedae-ro, Dongdaemun-gu, Seoul 02447, South Korea E-mail: imyj@khu.ac.kr
- *These authors contributed equally to this work as the first authors.
© 2026 Korean Society of Nursing Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution NoDerivs License (http://creativecommons.org/licenses/by-nd/4.0) If the original work is properly cited and retained without any modification or reproduction, it can be used and re-distributed in any format and medium.
- 1,612 Views
- 219 Download
Abstract
-
Purpose
- This study aimed to address the shift toward competency-based education and the planned 2028 “Integrated Nursing” National Licensing Examination (NLE), this study aimed to establish structural alignment among NLE domains, the seven integrated nursing competencies (INCs), and curriculum goals, with a particular focus on implementing symptom-based clinical reasoning (SBCR).
-
Methods
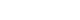
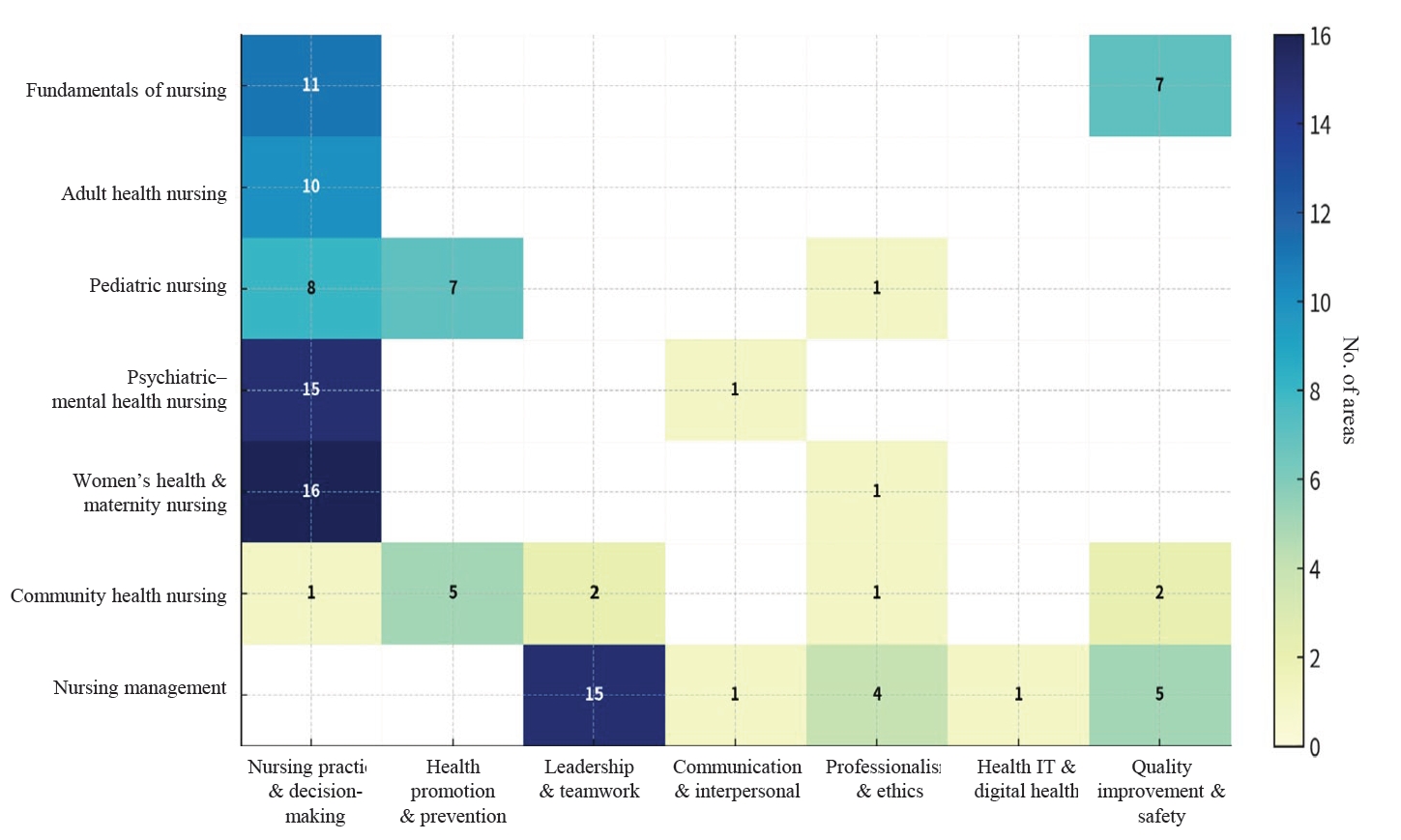
- This Delphi-based methodological study included seven content experts for content validity index (CVI) assessment and 24 nursing education experts who participated in a consensus workshop. The item-level CVI and the scale-level CVI/average were calculated to confirm the linkage between INCs and NLE domains. In addition, qualitative analysis of workshop materials and meeting records was conducted to derive 10 integrated learning topics and to develop an SBCR educational model for the key symptom of headache, grounded in Miller’s Clinical Competence Pyramid (levels 2–4).
-
Results
- The analysis confirmed the validity of integrating the INCs within the overall curriculum structure. The resulting framework delineates staged learning objectives and core clinical questions designed to systematically enhance clinical reasoning, promote safe nursing practice, and support professional reflection within a unified curriculum.
-
Conclusion
- This study provides a practical foundation for nursing curriculum redesign by facilitating a transition from fragmented, subject-based instruction to a holistic, patient-centered SBCR model. This approach aligns with the requirements of the integrated NLE and is expected to contribute to meaningful improvements in actual clinical competency.
서론
방법
1) 통합간호역량과 교과목별 국가시험 출제범위 연계
2) 연계 가능한 학습목표(학습주제) 도출
3) 연계 가능 학습목표(주제) 기반의 임상추론 교육방안 제시
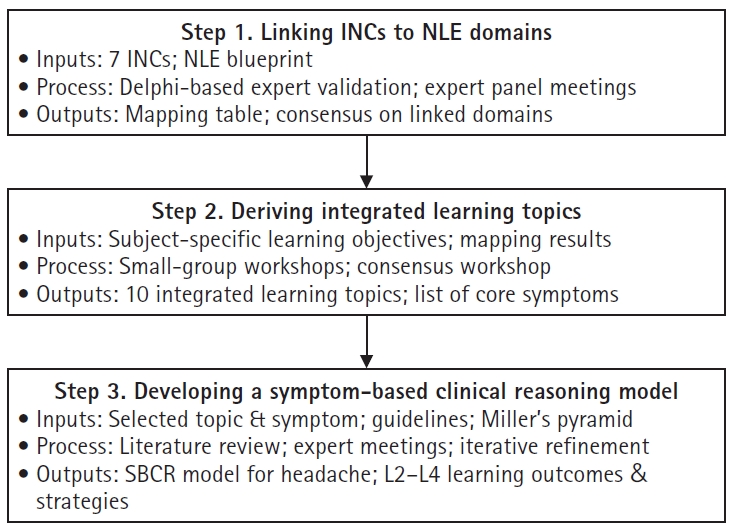
1) 통합간호역량과 교과목별 국가시험 출제범위 연계
2) 연계 가능 학습주제와 학습목표 도출
3) 연계 가능 학습목표(주제) 기반의 임상추론 교육방안 제시
결과
고찰
결론
-
Conflicts of Interest
No potential conflict of interest relevant to this article was reported.
-
Acknowledgements
We would like to express our sincere gratitude to the members of the Integrated National Licensing Examination Committee of the Korean Society of Nursing Science (Kisook Kim, Hye Young Kim, Heejung Kim, Ju-Hee Nho, Sunnam Park, Eunyoung Suh, Youngshin Song, Sujin Shin, Mi Yu, Hyang Yuol Lee, Sun Joo Jang, Yeonsoo Jang, Sangeun Jun, and Yeongmi Ha; names listed in Korean alphabetical order) for their participation and assistance, which enabled this study to proceed smoothly.
-
Funding
This study was supported by the 2025 Policy Research Grant of the Korean Society of Nursing Science and 2024 Sabbatical Year of Soonchunhyang University.
-
Data Sharing Statement
The datasets generated and/or analyzed during the current study are not publicly available due to privacy and ethical restrictions but are available from the corresponding author on reasonable request.
-
Author Contributions
Conceptualization or/and Methodology: all authors. Data curation or/and Analysis: all authors. Funding acquisition: none. Investigation: all authors. Project administration or/and Supervision: JIK, SY. Resources or/and Software: all authors. Validation: all authors. Visualization: all authors. Writing: original draft or/and Review & Editing: all authors. Final approval of the manuscript: all authors.
Article Information
- 1. Mani ZA. Transitioning to competency-based education in nursing: a scoping review of curriculum review and revision strategies. BMC Nurs. 2025;24(1):1111. https://doi.org/10.1186/s12912-025-03319-yArticlePubMedPMC
- 2. Muraraneza C, Mtshali GN. Planning reform to competency based curricula in undergraduate nursing and midwifery education: a qualitative study. Nurse Educ Today. 2021;106:105066. https://doi.org/10.1016/j.nedt.2021.105066ArticlePubMed
- 3. Goudreau J, Pepin J, Larue C, Dubois S; Descôteaux R, Lavoie P, et al. A competency-based approach to nurses' continuing education for clinical reasoning and leadership through reflective practice in a care situation. Nurse Educ Pract. 2015;15(6):572-578. https://doi.org/10.1016/j.nepr.2015.10.013ArticlePubMed
- 4. Muraraneza C, Mtshali NG, Mukamana D. Issues and challenges of curriculum reform to competency-based curricula in Africa: a meta-synthesis. Nurs Health Sci. 2017;19(1):5-12. https://doi.org/10.1111/nhs.12316ArticlePubMed
- 5. Kim KH, Kang SY, Kang YH, Kwon YR, Song YS, et al. A foundational study on developing test specifications based on an integrated model for the national nursing licensing examination [Internet]. Korea Health Personnel Licensing Examination Institute; 2021 [cited 2025 Nov 6]. Available from: https://www.kuksiwon.or.kr
- 6. Yu S, Kim HY, Kim JI, Lee J, Song JE, Lee HY. Core domains for pre-registered nurses based on program outcomes and licensing competencies. J Korean Acad Nurs. 2025;55(2):249-268. https://doi.org/10.4040/jkan.25017ArticlePubMed
- 7. Rojo J, Ramjan LM, Hunt L, Salamonson Y. Nursing students’ clinical performance issues and the facilitator’s perspective: a scoping review. Nurse Educ Pract. 2020;48:102890. https://doi.org/10.1016/j.nepr.2020.102890ArticlePubMed
- 8. Lee J, Lee YJ, Bae J, Seo M. Registered nurses’ clinical reasoning skills and reasoning process: a think-aloud study. Nurse Educ Today. 2016;46:75-80. https://doi.org/10.1016/j.nedt.2016.08.017ArticlePubMed
- 9. Menezes SS, Corrêa CG, Silva Rde C, Cruz Dde A. Raciocínio clínico no ensino de graduação em enfermagem: revisão de escopo [Clinical reasoning in undergraduate nursing education: a scoping review]. Rev Esc Enferm USP. 2015;49(6):1037-1044. https://doi.org/10.1590/S0080-623420150000600021Article
- 10. Kim JI. Visualization of unstructured personal narratives of perterm birth using text network analysis. Korean J Women Health Nurs. 2020;26(3):205-212. https://doi.org/10.4069/kjwhn.2020.08.08ArticlePubMedPMC
- 11. Miller GE. The assessment of clinical skills/competence/performance. Acad Med. 1990;65(9 Suppl):S63-S67. https://doi.org/10.1097/00001888-199009000-00045ArticlePubMed
- 12. Lynn MR. Determination and quantification of content validity. Nurs Res. 1986;35(6):382-385. https://doi.org/10.1097/00006199-198611000-00017ArticlePubMed
- 13. Polit DF, Beck CT. The content validity index: are you sure you know what’s being reported?: critique and recommendations. Res Nurs Health. 2006;29(5):489-497. https://doi.org/10.1002/nur.20147ArticlePubMed
- 14. American Association of Colleges of Nursing. The essentials: core competencies for professional nursing education [Internet]. American Association of Colleges of Nursing; 2021 [cited 2025 Nov 6]. Available from: https://www.aacnnursing.org/Portals/42/AcademicNursing/pdf/Essentials-2021.pdf
- 15. Simmons B. Clinical reasoning: concept analysis. J Adv Nurs. 2010;66(5):1151-1158. https://doi.org/10.1111/j.1365-2648.2010.05262.xArticlePubMed
- 16. Imanipour M, Ebadi A, Monadi Ziarat H, Mohammadi MM. The effect of competency-based education on clinical performance of health care providers: a systematic review and meta-analysis. Int J Nurs Pract. 2022;28(1):e13003. https://doi.org/10.1111/ijn.13003ArticlePubMed
- 17. Tan K, Chong MC, Subramaniam P, Wong LP. The effectiveness of outcome based education on the competencies of nursing students: a systematic review. Nurse Educ Today. 2018;64:180-189. https://doi.org/10.1016/j.nedt.2017.12.030ArticlePubMed
- 18. Giuffrida S, Silano V, Ramacciati N, Prandi C, Baldon A, Bianchi M. Teaching strategies of clinical reasoning in advanced nursing clinical practice: a scoping review. Nurse Educ Pract. 2023;67:103548. https://doi.org/10.1016/j.nepr.2023.103548ArticlePubMed
- 19. Tanner CA. Thinking like a nurse: a research-based model of clinical judgment in nursing. J Nurs Educ. 2006;45(6):204-211. https://doi.org/10.3928/01484834-20060601-04ArticlePubMed
- 20. Seo YH, Eom MR. The effect of simulation nursing education using the Outcome-Present State-Test model on clinical reasoning, the problem-solving process, self-efficacy, and clinical competency in Korean nursing students. Healthcare (Basel). 2021;9(3):243. https://doi.org/10.3390/healthcare9030243ArticlePubMedPMC
- 21. Cheng CY, Hung CC, Chen YJ, Liou SR, Chu TP. Effects of an unfolding case study on clinical reasoning, self-directed learning, and team collaboration of undergraduate nursing students: a mixed methods study. Nurse Educ Today. 2024;137:106168. https://doi.org/10.1016/j.nedt.2024.106168ArticlePubMed
- 22. Gonzalez L, Nielsen A, Lasater K. Developing students’ clinical reasoning skills: a faculty guide. J Nurs Educ. 2021;60(9):485-493. https://doi.org/10.3928/01484834-20210708-01ArticlePubMed
- 23. Xu HY, Wang XJ. Analysis of the current situation and factors influencing the clinical thinking ability of nursing undergraduates. Altern Ther Health Med. 2023;29(8):200-208.
- 24. Alberti S, Motta P, Ferri P, Bonetti L. The effectiveness of team-based learning in nursing education: a systematic review. Nurse Educ Today. 2021;97:104721. https://doi.org/10.1016/j.nedt.2020.104721ArticlePubMed
- 25. Gholami M, Changaee F, Karami K, Shahsavaripour Z, Veiskaramian A, Birjandi M. Effects of multiepisode case-based learning (CBL) on problem-solving ability and learning motivation of nursing students in an emergency care course. J Prof Nurs. 2021;37(3):612-619. https://doi.org/10.1016/j.profnurs.2021.02.010ArticlePubMed
- 26. Koukourikos K, Tsaloglidou A, Kourkouta L, Papathanasiou IV, Iliadis C, Fratzana A, et al. Simulation in clinical nursing education. Acta Inform Med. 2021;29(1):15-20. https://doi.org/10.5455/aim.2021.29.15-20ArticlePubMedPMC
- 27. Alharbi A, Nurfianti A, Mullen RF, McClure JD, Miller WH. The effectiveness of simulation-based learning (SBL) on students’ knowledge and skills in nursing programs: a systematic review. BMC Med Educ. 2024;24(1):1099. https://doi.org/10.1186/s12909-024-06080-zArticlePubMedPMC
- 28. Katebi MS, Ahmadi AA, Jahani H, Mohalli F, Rahimi M, Jafari F. The effect of portfolio training and clinical evaluation method on the clinical competence of nursing students. J Nurs Midwifery Sci. 2020;7(4):233-240. https://doi.org/10.4103/JNMS.JNMS_2_20Article
- 29. Oliver TL, Shenkman R, Diewald LK, Smeltzer SC. Reflective journaling of nursing students on weight bias. Nurse Educ Today. 2021;98:104702. https://doi.org/10.1016/j.nedt.2020.104702Article
References
Figure & Data
REFERENCES
Citations

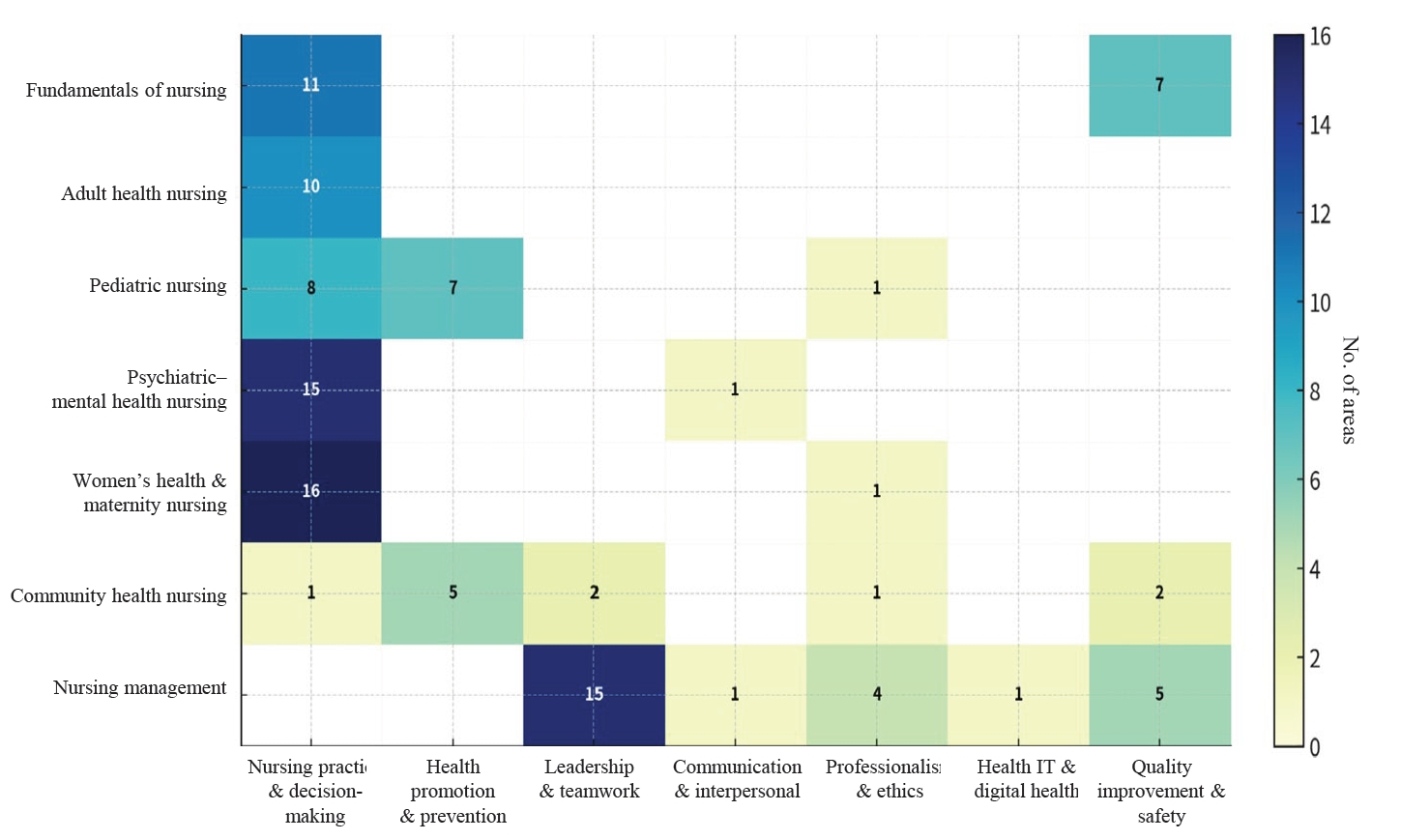
Fig. 1.
Fig. 2.
| Category | Topic | Learning objectives | Related courses |
|---|---|---|---|
| Symptom | Pain | Apply the nursing process to patients presenting with pain. | Women’s health, child health, fundamentals, adult health |
| Nausea and vomiting | Apply the nursing process to patients presenting with nausea and vomiting. | Women’s health, child health, fundamentals, adult health | |
| Sleep disturbance | Apply the nursing process to patients presenting with sleep disturbance. | Child health, fundamentals, adult health, psychiatric–mental health | |
| Violence exposure | Apply the nursing process to patients who have experienced violence. | Women’s health, child health, community health, psychiatric–mental health | |
| Disease | Impaired tissue perfusion | Apply the nursing process to patients with impaired tissue perfusion. | Women’s health, child health, fundamentals, adult health |
| Endocrine dysregulation | Apply the nursing process to patients with endocrine dysregulation. | Women’s health, child health, fundamentals, adult health | |
| Infectious health conditions | Apply the nursing process to patients with infectious health conditions. | Women’s health, child health, fundamentals, community health | |
| Chronic disease | Apply the nursing process to patients with chronic diseases. | Women’s health, child health, adult health, community health, psychiatric–mental health | |
| Fundamental care | Positioning | Apply appropriate positioning based on the patient’s clinical condition. | Women’s health, child health, fundamentals, adult health |
| Oral medication administration | Administer oral medications to address patients’ health problems and evaluate outcomes. | Women’s health, child health, fundamentals, adult health, community health, psychiatric–mental health |
| Nursing process (or clinical reasoning phase) | Miller’s learning level | Symptom-based clinical reasoning learning objective |
|---|---|---|
| Assessment (clinical information gathering) | L2 (Knows how) “Knows how to do it.” | Collect clinical information through history taking and physical examination of a patient with a headache. |
| Diagnosis (diagnostic reasoning) | L2 (Knows how) “Knows how to do it.” | Perform diagnostic reasoning by synthesizing the characteristics of the headache and clinical clues. |
| Planning (presenting nursing interventions) | L3 (Shows how) “Can show how.” | Present appropriate nursing intervention plans based on the results of the diagnostic reasoning for the headache patient. |
| Implementation (applying nursing interventions) | L4 (Does) “Does it in real clinical practice.” | Apply interventions with an empathetic attitude, respecting the headache patient’s subjective experience. |
| Evaluation (judging the appropriateness of interventions and reflection) | L4 (Does) “Does it in real clinical practice.” | Judge the appropriateness of interventions based on changes in the headache patient’s symptoms and reactions. |
| Learning objectives | Integrated nursing competency | Clinical reasoning (algorithm) questions |
|---|---|---|
| 1. Collect clinical information through history-taking and physical examination for a patient with headache, including comprehensive history of pain pattern (PQRST), triggers (stress, food, hormonal cycle), lifestyle, and work environment. | Communication and interpersonal | What is the patient’s most critical problem, and what information is needed to address it? |
| 1) What are the red flag signs suggesting life‑threatening headaches? | ||
| • Any unusually frequent or unusually severe headaches? | ||
| • Have you had this type of headache before? | ||
| • On a scale from 0 (no pain) to 10 (worst pain ever), how severe is the pain? | ||
| • Do you have a history of recent trauma to the head of loss of consciousness? | ||
| 2) After determining that a headache is not serious, how can I narrow down the cause? | ||
| • What are the pain characteristics, aggravating factors, and duration? | ||
| • Any family history of headache? | ||
| • Any prodrome or aura signs before the headache? | ||
| 3) Physical examination | ||
| • Inspection: If ataxic gait, uncoordinated movements, or changes in consciousness are present, recognize that this is an emergency requiring neurological assessment. Refer to the emergency center. | ||
| • Take vital signs and test neck stiffness for meningitis. | ||
| • Palpate and percuss the skull | ||
| 4) Consider laboratories studies such as hemoglobin (anemia), WBC (infection), etc. | ||
| 2. Perform diagnostic reasoning by integrating headache characteristics and clinical clues to infer causes and identify priority nursing problems (e.g., chronic pain, ineffective coping) and assess impact on daily life and quality of life. | Nursing practice and decision-making | Based on the collected data, what is the priority nursing problem and what key cues support it? |
| • What other symptoms does the patient have? | ||
| • Do headache features suggest migraine (nausea, vomiting, photophobia, phonophobia). | ||
| • Are there aura symptoms (visual, sensory, language) indicating migraine with aura. | ||
| • Does migraine affect daily life? | ||
| 3. Propose appropriate nursing interventions based on diagnostic reasoning, collaborate with other professionals as needed, and develop a self‑management education plan that includes nonpharmacologic interventions (e.g., lifestyle modification) and correct use of analgesics (e.g., acetaminophen). | Health promotion and prevention | What are the priority nursing interventions to resolve the migraine? |
| Leadership and teamwork | • Can environmental or dietary triggers be modified? | |
| • What medication precautions should the patient be taught when using migraine treatments? | ||
| • Are there areas that require collaboration with other specialties? | ||
| 4. Apply interventions with respect for the patient’s subjective experience, using an empathic approach while delivering the planned self‑management education (e.g., relaxation therapy, limiting caffeine). | Professionalism and ethics | Can you demonstrate empathy and assess the patient’s capacity to manage migraine and pain control? |
| • Does the patient recognize any family history of migraine? | ||
| • Does the patient understand the need for a quiet, dark environment to help control migraine? | ||
| 5. Evaluate interventions by monitoring symptom changes and patient‑reported responses using health IT and digital health tools; assess adherence and effectiveness (headache frequency and intensity), and revise the care plan if goals are unmet. | Quality improvement and safety | What is the key evidence for determining whether the intervention was successful? |
| Health IT and digital health | • What evidence can confirm the success of the nursing intervention? | |
| • If nursing goals for reducing environmental triggers or implementing lifestyle changes are not met, which steps of the plan should be revised? |
IT, information technology; PQRST, Provocation/Palliation, Quality, Region/Radiation, Severity, and Timing; WBC, white blood cell.
 KSNS
KSNS
 Submit an article
Submit an article
 ePub Link
ePub Link Cite
Cite