Articles
- Page Path
- HOME > J Korean Acad Nurs > Volume 54(4); 2024 > Article
-
Research Paper
간호대학생의 투약안전을 위한 점진적 시뮬레이션 교육프로그램 개발 및 효과 -
정세영
 , 김은영
, 김은영
- Development and Effectiveness of Progressive Simulation Education Program on Medication Safety for Nursing Students
-
Se-Young Jung
 , Eun-Young Kim
, Eun-Young Kim
-
Journal of Korean Academy of Nursing 2024;54(4):563-576.
DOI: https://doi.org/10.4040/jkan.24054
Published online: October 14, 2024
동아대학교 간호학부
College of Nursing, Dong-A University, Busan, Korea
- Address reprint requests to : Kim, Eun-Young College of Nursing, Dong-A University, Daesingongwon-ro 32, Seo-gu, Busan 49201, Korea Tel: +82-51-240-2785 Fax: +82-51-240-2695 E-mail: eykim@dau.ac.kr
• Received: April 29, 2024 • Revised: May 27, 2024 • Accepted: July 24, 2024
© 2024 Korean Society of Nursing Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution NoDerivs License (http://creativecommons.org/licenses/by-nd/4.0) If the original work is properly cited and retained without any modification or reproduction, it can be used and re-distributed in any format and medium.
Figure & Data
REFERENCES
Citations
Citations to this article as recorded by 

- Safety-centered simulation education using the 360-degree video room of errors: A mixed-methods study
Jiyoung Kim, Yeji Kim, Hyunji Park, Jiyeong Won, Jiwon Yun, Yuran Lee
Clinical Simulation in Nursing.2026; 111: 101899. CrossRef
Development and Effectiveness of Progressive Simulation Education Program on Medication Safety for Nursing Students
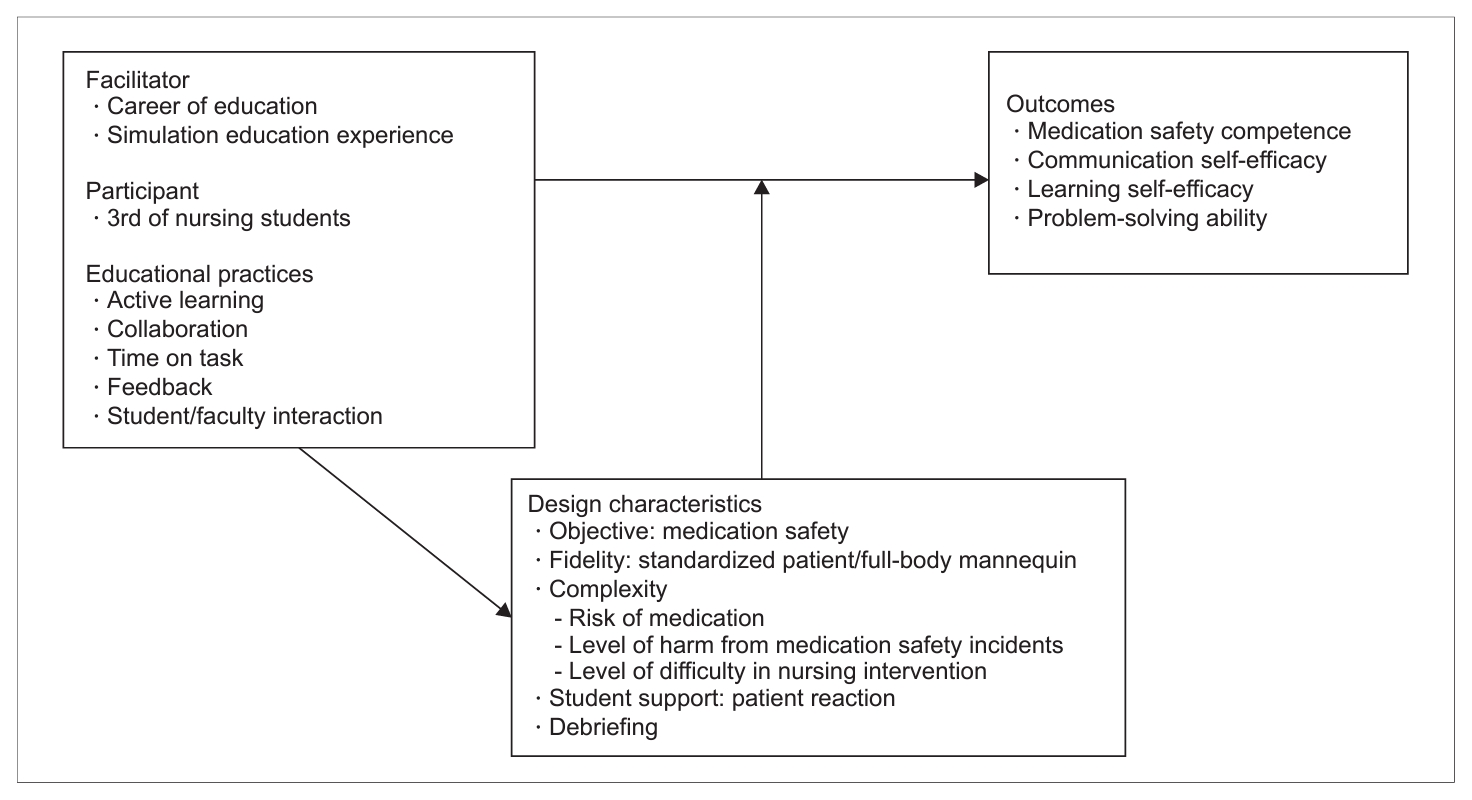
Fig. 1. Conceptual framework of the progressive simulation education program.
Fig. 1.
Development and Effectiveness of Progressive Simulation Education Program on Medication Safety for Nursing Students
| Scenarios | Learning objectives | Situations | Role and expected learner behaviors |
|---|---|---|---|
| Scenario 1 | The nurses can identify medication safety-related problem situations (near-misses). | • Hospital day 1 | • An evening-shift nurse (student) detects an error using a patient identification bracelet (ID band) and asks open-ended questions before administering the medication. |
| • A medication error may occur if an evening-shift nurse does not accurately check a patient with the same name during the medication preparation stage when administering fluid that the previous shift nurse prepared in advance for a patient with the same name. | • If a nurse cannot detect the error, the nursing manager provides a clue. | ||
| Scenario 2 | The nurses can identify and respond to problem situations related to medication safety (prescription errors/none). | • Hospital day 2 | • An evening-shift nurse (student) discovers that the patient took oral drugs whose administration was prohibited before the CT scan. |
| • A situation in which a patient’s scheduled upper abdominal CT scan was delayed because a doctor’s incorrect prescription instructions caused the previous shift nurse to incorrectly administer medication to the patient that should have been stopped prior to the CT scan. | • If a nurse cannot detect the error, the nursing manager provides a clue. | ||
| Scenario 3 | The nurses can identify and respond to crisis situations related to medication safety (adverse events/moderate). | • Hospital day 3 | • An evening-shift nurse (student) suspects that the patient is suffering from hypoglycemic shock and responds to it. |
| • A situation in which serious damage occurred because a day-shift nurse administered medication to the patient using the wrong dosage and a route that was inconsistent with a doctor’s prescription instructions. | • If the nurse cannot detect the error, the nursing manager provides a clue. |
| Sessions | Sequences | Contents | Time (min) |
|
|---|---|---|---|---|
| Time | Cumulative | |||
| Session 1 | Pre-learning | • Medication safety–related knowledge (lecture) | 20 | 65 |
| - Basic principles of medication administration, types of patient safety accidents, activities to prevent medication errors | ||||
| Pre-briefing | • Guide to simulation practice environment and process | 15 | ||
| • Introduction to scenario case outlines | ||||
| • Introduction to Scenario 1 situation | ||||
| • Identifying nursing issues and setting priorities | ||||
| • Assigning simulation roles | ||||
| Simulation run | • Detecting and dealing with near-misses (SP, full-body mannequin) | 10 | ||
| • Nursing performance evaluation | ||||
| Debriefing | • Reflection and feedback | 20 | ||
| Session 2 | Pre-learning | • Medication safety–related knowledge (lecture) | 20 | 80 |
| - Medication process, types of medication errors, communicating patient safety accidents (SBAR) | ||||
| Pre-briefing | • Introduction to Scenario 2 situation | 15 | ||
| • Identifying nursing issues and setting priorities | ||||
| • Assigning simulation roles | ||||
| Simulation run | • Identifying and dealing with prescription errors (SP, full-body mannequin) | 15 | ||
| • Nursing performance evaluation | ||||
| Debriefing | • Reflection and feedback | 30 | ||
| Session 3 | Pre-learning | • Medication safety–related knowledge (lecture) | 20 | 95 |
| - High-alert medication management, patient safety accident reporting, patient safety accident analysis | ||||
| Pre-briefing | • Introduction to Scenario 3 situation | 15 | ||
| • Identifying nursing problems and setting priorities | ||||
| • Assigning simulation roles | ||||
| Simulation run | • Detecting and dealing with adverse events (SP, full-body mannequin) | 20 | ||
| • Nursing performance evaluation | ||||
| Debriefing | • Reflection and feedback | 40 | ||
| Variables | Categories | Exp. (n = 20) |
Cont. (n = 20) |
t or χ2 | p |
|---|---|---|---|---|---|
| n (%) or M ± SD | |||||
| General characteristics | |||||
| Age (yr) | 21.4 ± 1.23 | 21.5 ± 1.10 | – 0.41 | .686 | |
| Gender | Woman | 18 (90.0) | 19 (95.0) | < .999 |
|
| Man | 2 (10.0) | 1 (5.0) | |||
| Religion | Yes | 6 (30.0) | 4 (20.0) | 0.53 | .465 |
| No | 14 (70.0) | 16 (80.0) | |||
| Previous semester grade | ≥ 3.5 | 9 (45.0) | 12 (60.0) | 0.90 | .342 |
| < 3.5 | 11 (55.0) | 8 (40.0) | |||
| Experience of healthcare service | Have | 3 (15.0) | 3 (15.0) | < .999 |
|
| Haven’t | 17 (85.0) | 17 (85.0) | |||
| Satisfaction of major | Above high | 12 (60.0) | 15 (75.0) | 1.03 | .311 |
| Middle or less | 8 (40.0) | 5 (25.0) | |||
| Satisfaction of clinical practice | Above high | 11 (55.0) | 10 (50.0) | 0.10 | .752 |
| Middle or less | 9 (45.0) | 10 (50.0) | |||
| Reasons for entering nursing college | Easy employment | 11 (55.0) | 10 (50.0) | 2.56 | .333 |
| Aptitude | 5 (25.0) | 2 (10.0) | |||
| Recommendation | 4 (20.0) | 8 (40.0) | |||
| Type of apply for a job | Hospitals | 18 (90.0) | 19 (95.0) | 0.36 | .548 |
| Other than hospitals | 2 (10.0) | 1 (5.0) | |||
| Medication safety competence | 119.70 ± 10.68 | 120.05 ± 11.79 | – 0.10 | .922 | |
| Communication self-efficacy | 86.55 ± 11.86 | 83.80 ± 11.96 | 0.73 | .470 | |
| Learning self-efficacy | 56.90 ± 5.71 | 57.10 ± 4.23 | – 0.13 | .901 | |
| Problem-solving ability | 108.75 ± 14.41 | 112.00 ± 11.13 | – 0.80 | .430 | |
| Variables | Pre-test |
Post-test |
Difference |
t | p | |||
|---|---|---|---|---|---|---|---|---|
| Exp. (n = 20) | Cont. (n = 20) | Exp. (n = 20) | Cont. (n = 20) | Exp. (n = 20) | Cont. (n = 20) | |||
| Medication safety competence | 119.70 ± 10.68 | 120.05 ± 11.79 | 144.90 ± 10.47 | 132.55 ± 10.96 | 25.20 ± 10.05 | 12.50 ± 8.56 | 4.30 | < .001 |
| Communication self-efficacy | 86.55 ± 11.86 | 83.80 ± 11.96 | 99.80 ± 10.28 | 87.35 ± 12.23 | 13.25 ± 7.44 | 3.55 ± 7.50 | 4.11 | < .001 |
| Learning self-efficacy | 56.90 ± 5.71 | 57.10 ± 4.23 | 77.40 ± 4.45 | 72.78 ± 4.97 | 20.50 ± 4.37 | 15.68 ± 4.65 | 3.01 | .005 |
| Problem-solving ability | 108.75 ± 14.41 | 112.00 ± 11.13 | 124.40 ± 12.48 | 114.00 ± 9.49 | 15.65 ± 7.60 | 2.00 ± 5.42 | 6.54 | < .001 |
Table 1. Scenario Progression
CT = Computed tomography; ID = Identification.
Table 2. Summary of the Progressive Simulation Education Program
SBAR = Situation, background, assessment, recommendation; SP = Simulated patient.
Table 3. Homogeneity Test of General Characteristics and Dependent Variables of Participants (N = 40)
Fisher’s exact test. Cont. = Control group; Exp. = Experimental group; M = Mean; SD = Standard deviation.
Table 4. Effects of the Progressive Simulation Education Program (N = 40)
Cont. = Control group; Exp. = Experimental group.
 KSNS
KSNS
 Submit an article
Submit an article

 ePub Link
ePub Link Cite
Cite